Skin Issues and Diabetes
Diabetes can affect the skin in many ways. Proper care and early attention can keep your skin healthy and prevent complications.
This content is not medical advice. Always consult your endocrinologist, doctor or diabetes care team before making any changes to your diabetes treatment or daily management.
Taking Care of Your Skin with Diabetes
Skin problems are common among people living with diabetes. High blood sugar levels can lead to dryness, slow healing, and an increased risk of infections. Additionally, everyday diabetes management such as using pumps, continuous glucose monitors (CGMs), and adhesive patches can sometimes cause irritation or allergic reactions.
Good skin care and early recognition of changes are key to preventing more serious complications. Simple habits, like daily moisturizing, staying hydrated, and checking your skin regularly, can make a big difference.
Below are some of the most common skin-related challenges for people with diabetes and how to manage them effectively:
Dry Skin and Diabetes
Dry or itchy skin is one of the most common skin problems for people living with diabetes. High blood glucose levels can cause the body to lose fluids, leading to dehydration and dry skin. Over time, this dryness can make the skin more likely to crack, itch, or become infected.
Why Diabetes Causes Dry Skin?
When blood sugar levels stay high, the body tries to get rid of excess glucose through urine. This process draws water from the body, leading to dehydration. Poor circulation and nerve damage (neuropathy) can also reduce the amount of sweat and natural oils that keep the skin soft and healthy especially on the legs, feet, and hands.
Tips for Preventing and Treating Dry Skin
-
Moisturize daily, especially after bathing, to lock in moisture.
-
Use gentle, fragrance-free soaps and lotions to avoid irritation.
-
Avoid very hot showers or baths, as they can dry out your skin.
-
Drink plenty of water throughout the day to stay hydrated.
-
Use a humidifier during winter or in dry environments.
-
Check your feet and legs daily for cracks, redness, or signs of infection.

When to Contact Your Doctor?
If you notice persistent dryness, cracking, or wounds that don’t heal, or if the area becomes red, swollen, or painful, contact your healthcare provider. These can be signs of infection or circulation problems that require medical attention.

Skin Infections and Diabetes
People living with diabetes are more likely to develop skin infections, especially when blood glucose levels are high. High sugar in the blood and tissues creates an environment where bacteria and fungi can grow more easily. Minor cuts, blisters, or irritation can quickly turn into infections if not treated promptly.
Common Types of Skin Infections
Bacterial infections: such as styes, boils, infected hair follicles, or inflamed skin around the nails. These are often caused by Staphylococcus (Staph) bacteria and can make the skin red, swollen, and painful.
Fungal infections: yeast infections like Candida albicans thrive in warm, moist areas — under the breasts, between fingers and toes, around the groin, or in skin folds. Common symptoms include redness, itching, and small blisters or scales.
Itchy rashes and athlete’s foot: frequent among people who wear tight shoes or stay in humid environments.
Signs of Infection to Watch For
-
Redness, warmth, or swelling
-
Pain or tenderness
-
Pus or drainage
-
Itching or burning
-
Fever or fatigue (if infection spreads)
Preventing Skin Infections
Keep blood glucose levels within target range. High blood sugar weakens your body’s natural defenses.
Maintain good hygiene. Bathe regularly and dry your skin carefully, especially between toes and skin folds.
Treat cuts and scratches immediately. Clean with mild soap and water, then apply an antiseptic or antibiotic cream.
Avoid sharing towels or personal items. This helps prevent bacterial or fungal spread.
Wear loose, breathable clothing. Helps reduce sweat and moisture buildup.
Check your feet daily. Even small sores can become infected quickly.
When to See Your Doctor?
If you notice any signs of infection: redness, warmth, swelling, pain, or pus contact your doctor or diabetes care team immediately. Early treatment helps prevent complications like cellulitis or ulcers.
Slow Wound Healing and Diabetes
For people living with diabetes, even small cuts or blisters can take longer to heal. High blood glucose levels can affect circulation and nerve function, reducing the body’s ability to repair itself. Slow healing increases the risk of infections and, in severe cases, ulcers, especially on the feet and lower legs.
Why Wounds Heal Slowly?
-
Reduced blood flow: High blood sugar can damage blood vessels, slowing oxygen and nutrient delivery to the wound.
-
Nerve damage (neuropathy): When you can’t feel pain, small cuts or blisters may go unnoticed and untreated.
-
Weakened immune response: Elevated glucose levels impair the body’s ability to fight off bacteria and infections.
-
Dry skin and poor hydration: These can lead to cracks that open the skin to infection.
How to Help Wounds Heal Faster?
- Keep wounds clean and covered. Wash gently with mild soap and water, then use a sterile dressing.
-
Don’t pop blisters or peel scabs. Let the skin heal naturally.
-
Keep blood glucose levels in target range. This helps your body heal faster.
-
Avoid tight shoes or socks. Friction can worsen sores or delay healing.
-
Eat a balanced diet. Protein, vitamins C and E, and zinc support healing.
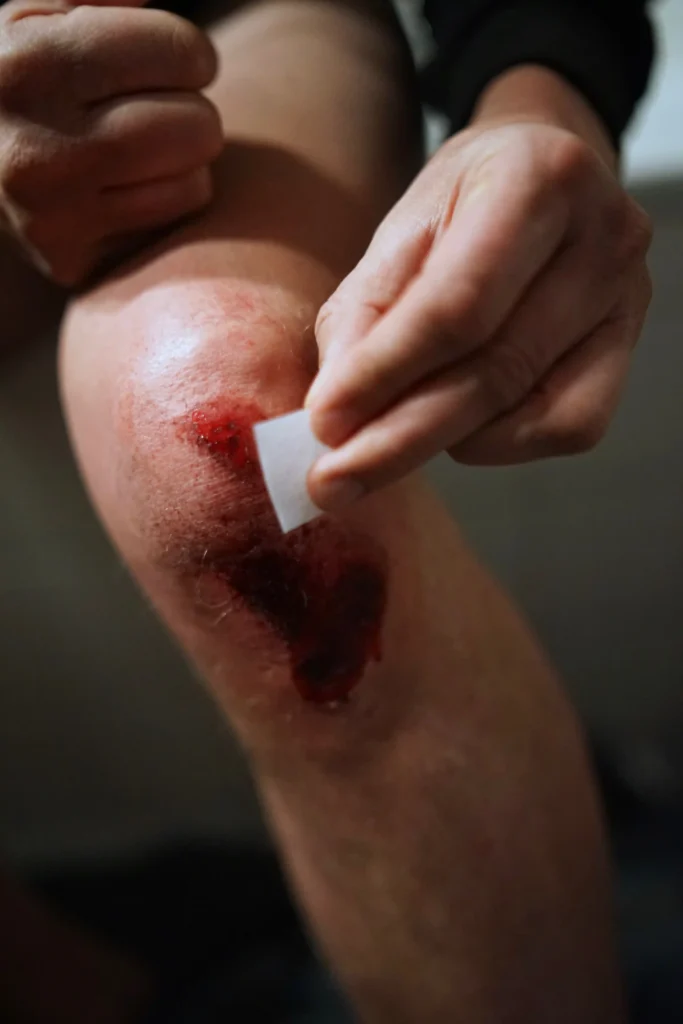
When to See Your Doctor?
If a cut, blister, or sore doesn’t start healing within a few days or if it becomes red, swollen, painful, or has pus contact your doctor or diabetes care team immediately. Prompt medical attention can prevent serious complications like ulcers or infections that spread deeper into the skin.
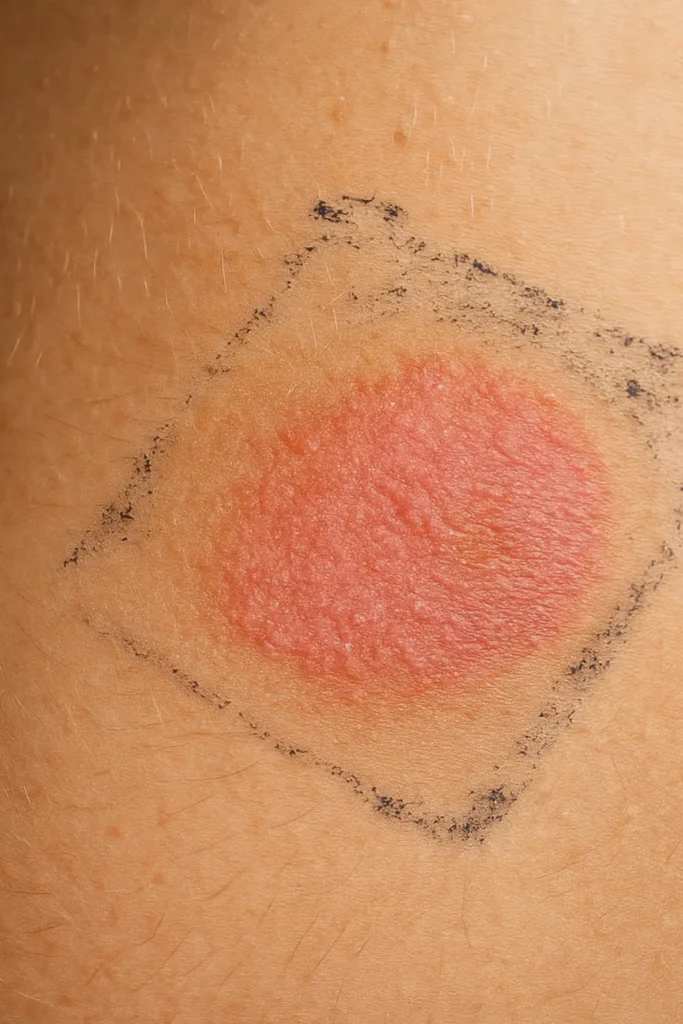
Skin irritation from diabetes devices
Wearing insulin pumps, continuous glucose monitors (CGMs), and adhesive patches can sometimes cause skin irritation, redness, or allergic reactions. These issues are often caused by friction, sweat, or sensitivity to the adhesive used in the devices.
How to Reduce Irritation?
Prepare your skin before applying a device. Wash the area with mild soap and let it dry completely before attaching the device.
Use barrier wipes or protective film. These create a thin layer between your skin and the adhesive, reducing friction and irritation.
Rotate application sites. Change where you place your device regularly to give your skin time to recover.
Moisturize gently after removal. Apply a fragrance-free lotion once you remove the device to soothe and rehydrate the skin.
Avoid applying to irritated or broken skin. Wait until the area heals completely before reattaching your device.
Try hypoallergenic adhesives. Some manufacturers offer options designed for sensitive skin.
If redness, itching, or rash persists, talk to your doctor or dermatologist. They can recommend protective creams or topical treatments to help your skin heal and reduce future irritation.
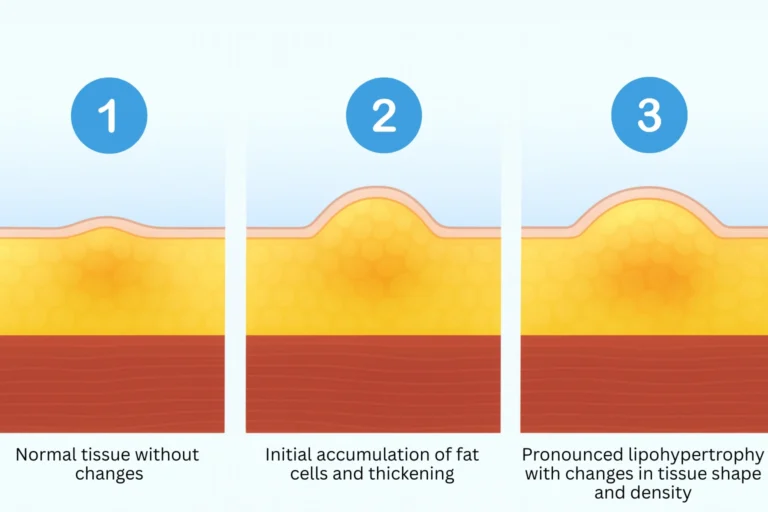
Injection Site Issues
Frequent insulin injections can sometimes cause skin problems such as redness, bruising, or thickened areas under the skin (lipohypertrophy). These changes happen when insulin is injected in the same spot repeatedly.
How to prevent it:
Rotate your injection sites — switch between different areas of the abdomen, thighs, and arms.
Avoid injecting into scarred or thickened skin.
Use a new needle every time to prevent irritation or infection.
If you notice lumps, dents, or persistent redness, talk to your healthcare provider, they can help you adjust your injection technique.
Join as a T1D Warrior

Our T1D Warriors are children, parents of children with diabetes, and individuals living with type 1 diabetes who share their personal experiences to inspire and support others. Every story, every blog post, and every piece of advice you find here comes from someone who has truly lived it — with honesty, courage and a whole lot of heart. Together, we’re building a community where real-life experience truly makes a difference.
Want to inspire others with your T1D journey? Become a T1D Warrior and share your story.
