The Honeymoon Phase
The honeymoon phase in type 1 diabetes is a period after diagnosis when the pancreas still produces a small amount of insulin. During this time, blood sugar control may be easier, but the phase is temporary and gradually comes to an end.
This content is not medical advice. Always consult your endocrinologist, doctor or diabetes care team before making any changes to your diabetes treatment or daily management.
The Honeymoon Phase in Type 1 Diabetes
After being diagnosed with type 1 diabetes, some people experience a unique period known as the honeymoon phase — a short-lived stage when your body still produces some of its own insulin, making diabetes care less demanding than it will be later.
For most people, this is partial remission, meaning you still need small doses of insulin, but much less than at diagnosis. In rare cases, it can be complete remission, where no insulin is needed for a period of time.
The name “honeymoon” comes from the idea that things feel calmer and less complicated during this time. But, just like a real honeymoon, it doesn’t last forever. While it’s happening, your insulin needs are lower, your blood sugar may be easier to keep within range, and you might even feel like your diabetes has become more manageable. Still, type 1 diabetes is present, and the honeymoon phase is only a temporary pause before the condition requires full, ongoing management again.
How the Honeymoon Phase Starts?
Type 1 diabetes happens when the immune system mistakenly attacks the beta cells in the pancreas the cells responsible for making insulin. By the time symptoms appear and a diagnosis is made, most of these cells have already been destroyed, but a small number are still active.
When you start insulin treatment, your blood sugar levels improve, and the pressure on those remaining beta cells decreases. This “rest” allows them to keep producing some insulin for a while, helping your body work alongside the insulin you inject. As a result, your overall insulin needs drop, and controlling blood sugar becomes easier at least temporarily.
For many people, this smoother control begins within weeks or months after diagnosis. It’s the combination of medical treatment and the pancreas’ remaining ability that makes this phase possible.
What’s the Difference Between Partial and Complete Remission?
Not everyone experiences the honeymoon phase in the same way. For some, it’s a partial remission, while for others much less commonly it can be a complete remission.
Partial remission means your pancreas is still making some insulin, but not enough to keep your blood sugar within range on its own. You still need insulin therapy, just in much smaller doses than at diagnosis. Blood sugar levels are generally easier to manage during this stage.
Complete remission means your pancreas is producing enough insulin to maintain healthy blood sugar levels without the need for insulin injections or other diabetes medication. This is rare and usually doesn’t last long.
In both cases, remission is temporary. The immune system continues to attack the insulin-producing beta cells, and over time, your body will again require full insulin therapy
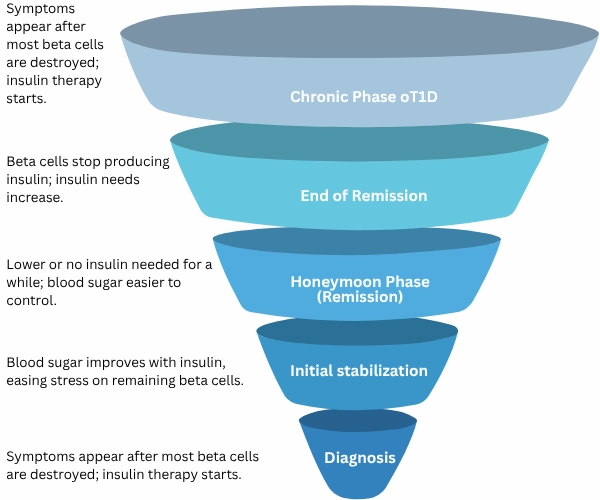
End of the Honeymoon Phase – Complete Dependence on Insulin
Eventually, the honeymoon phase comes to an end. The immune system continues to destroy the remaining insulin-producing beta cells in the pancreas until there are too few left to produce meaningful amounts of insulin.
At this point:
Blood sugar becomes harder to manage without adequate insulin therapy.
Insulin doses gradually increase to meet the body’s needs.
Fluctuations in blood sugar may become more frequent if doses aren’t well adjusted.
The end of remission doesn’t mean you’ve done anything wrong — it’s simply the natural course of type 1 diabetes. With the right insulin regimen, regular blood sugar monitoring, and ongoing support, you can still maintain good control and live a full, active life.
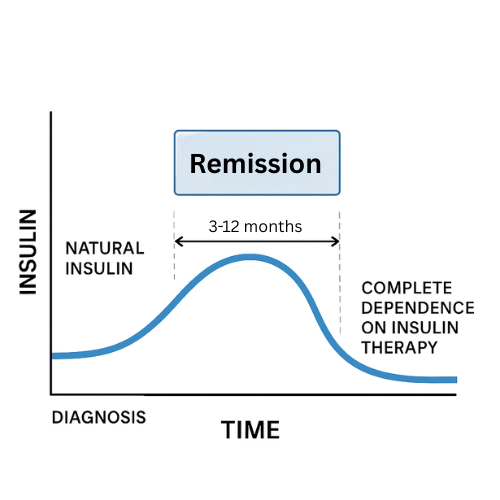
According to research, the remission phase in type 1 diabetes can last from a few weeks to an average of 3–12 months. In rare cases, remission has been documented to last several years, but such instances are exceptions. Duration depends on various factors, including age at diagnosis, preserved beta cell function, blood glucose control, and the presence of autoantibodies.
Chronic Phase – Living Beyond the Honeymoon
When the remission (honeymoon) phase ends, the body no longer produces enough of its own insulin, leading to complete dependence on insulin therapy. From this point onward, type 1 diabetes becomes a lifelong condition that requires daily management.
This stage focuses on:
Consistent insulin therapy – adjusting doses based on blood glucose readings, meals, and activity levels.
Regular monitoring – daily blood glucose checks, CGM use, and periodic HbA1c testing.
Healthy lifestyle – balanced nutrition, regular physical activity, and stress management.
Complication prevention – eye exams, kidney function monitoring, and foot care to catch and manage issues early.
With a well-structured care plan and ongoing support, people with type 1 diabetes can maintain good health and lead active, fulfilling lives.
Join as a T1D Warrior

Our T1D Warriors are children, parents of children with diabetes, and individuals living with type 1 diabetes who share their personal experiences to inspire and support others. Every story, every blog post, and every piece of advice you find here comes from someone who has truly lived it — with honesty, courage and a whole lot of heart. Together, we’re building a community where real-life experience truly makes a difference.
Want to inspire others with your T1D journey? Become a T1D Warrior and share your story.
